Réduction mammaire à Paris : Prise en charge, prix et avant après
Réduction mammaire : quels sont les avantages ?
La réduction mammaire, ou mammoplastie de réduction, est bien plus qu’un acte esthétique, c’est un acte de chirurgie réparatrice qui transforme en profondeur le quotidien des patientes. En réduisant à la fois le volume des seins et leur ptose (affaissement), elle permet de retrouver une poitrine plus légère, plus haute, et mieux proportionnée. Au-delà de l’aspect visuel, les bienfaits physiques et psychologiques sont nombreux :
- Diminution des douleurs chroniques (dos, épaules, nuque) grâce à l’allègement du poids mammaire.
- Amélioration de la posture et du confort général, avec une sensation de libération corporelle.
- Facilité retrouvée pour pratiquer une activité physique, sans gêne ni inconfort.
- Réduction des irritations cutanées sous les seins, souvent causées par le frottement ou l’humidité.
- Résultat esthétique complet, avec une poitrine redessinée, remontée et mieux proportionnée à la silhouette.
- Confiance en soi renforcée, grâce à une silhouette plus harmonieuse et une poitrine plus légère et remontée.
La réduction mammaire apporte ainsi une réponse concrète aux douleurs physiques et aux complexes liés à une forte poitrine, pour un mieux-être durable.
Réduction mammaire définition : en quoi ça consiste ?
La réduction mammaire, aussi appelée plastie mammaire de réduction, est une intervention chirurgicale qui vise à diminuer le volume des seins tout en améliorant leur forme et leur position. Elle s’adresse principalement aux femmes souffrant d’une poitrine trop volumineuse, souvent source de douleurs dorsales, de gêne dans la vie quotidienne ou de complexes esthétiques.
L’intervention consiste à retirer l’excès de glande mammaire, de graisse et parfois de peau, généralement dans la partie inférieure du sein. Le tissu restant est ensuite remodelé pour créer une poitrine plus ferme, plus haute et plus harmonieuse avec la silhouette. Le mamelon et l’aréole sont repositionnés vers une zone anatomiquement plus naturelle, au sommet du nouveau galbe du sein.
Il existe plusieurs techniques chirurgicales selon le degré de réduction nécessaire et l’élasticité de la peau. Dans la majorité des cas, les cicatrices sont en forme de T inversé (ou « ancre marine »), associant une incision verticale et une incision horizontale dans le pli sous-mammaire. Chez certaines patientes plus jeunes ou présentant une hypertrophie modérée, une cicatrice verticale seule peut suffire.
Dans de très rares cas, nous pouvons même proposer une réduction mammaire par lipoaspiration permettant d’obtenir un résultat avec des cicatrices inférieures à 1 cm.
Cette opération apporte un réel confort physique et une amélioration esthétique durable, tout en conservant, dans la plupart des cas, la sensibilité du sein et la possibilité d’allaiter.
Réduction des seins : déroulement de l’intervention
Si vous avez des antécédents familiaux de cancer du sein, une mammographie et une échographie peuvent vous être demandées.
La réduction mammaire est réalisée sous anesthésie générale. Ceci nécessite une consultation pré-anesthésique au minimum 48 h avant l’intervention.
Dans la majorité des cas, l’intervention est réalisée en hospitalisation conventionnelle (entrée à 13h sortie à 11 h le lendemain) mais peut parfaitement s’envisager en chirurgie ambulatoire (entrée à 8h, sortie à 18h) .
L’opération est peu douloureuse mais les soins post-opératoires nécessitent d’arrêter son activité professionnelle pendant 7 à 21 jours en fonction de la pénibilité de votre emploi.
Notre technique opératoire spécifique de réduction mammaire
Contrairement à la majorité de nos confrères français qui utilisent une technique à pédicule supérieur, nous utilisons une technique opératoire spécifique (technique du pédicule supéro-interne) décrite par une chirurgienne canadienne (Elisabeth Hall-Findlay).
Cette technique à l’immense avantage de ne pas séparer l’aréole et le mamelon de la glande sous jacente. Ceci permet :
- d’éviter quasiment tout risque de nécrose de l’aréole et du mamelon (5% des cas avec la technique à pédicule supérieur)
- d’améliorer fortement la sensibilité post opératoire de l’aréole et du mamelon et préserver cette zone érogène
de pouvoir envisager un allaitement après une réduction mammaire (impossible avec la technique à pédicule supérieure).
Cette technique permet aussi de limiter les décollements de tissus importants et permettre une chirurgie de réduction mammaire en ambulatoire sans pose de drain de Redon
Questions / Réponses sur la réduction mammaire
Quelles sont les complications possibles d’une réduction mammaire ?
La complication principale est l’altération de la sensibilité de l’aréole et du mamelon. Celle-ci peut persister à long terme, mais le risque est fortement réduit lorsque nous réalisons la technique chirurgicale du pédicule supéro-interne.
Un hématome ou caillot de sang peut survenir le soir de l’intervention mais ceci est extrêmement rare.
En cas de seins très volumineux, une souffrance de l’aréole peut survenir dont 5% des cas nécessiteront une greffe de l’aréole pendant ou le lendemain de l’intervention.
Réduction mammaire cicatrices : combien de temps après intervention ?
Les cicatrices après une réduction mammaire sont initialement épaisses et inflammatoires les 3 premiers mois, puis diminuent fortement jusqu’à 18 mois après l’intervention.
Réduction mammaire douleur : combien de temps durent les douleurs ?
La réduction mammaire est généralement bien tolérée sur le plan de la douleur. Les sensations post-opératoires sont souvent décrites comme des tiraillements ou une gêne modérée, plutôt qu’une douleur intense. Cette intervention n’affecte pas les muscles, ce qui limite considérablement l’inconfort. Des antalgiques adaptés sont prescrits pour soulager les premières sensations, et la majorité des patientes retrouve une bonne autonomie en quelques jours. Quelques brûlures légères au niveau des cicatrices peuvent persister temporairement, mais elles s’atténuent progressivement.
Diminution des seins : Quels sont les soins post-opératoires après l’intervention ?
Les soins post-opératoires sont relativement simples.
Le lendemain de l’intervention, les drains vous sont retirés par l’infirmière et les soins sont effectués après la douche.
Ils consistent en une désinfection de la cicatrice suivie de la mise en place de pansements ou de compresses dans le soutien gorge de sport.
Ces soins sont répétés tous les jours à votre domicile pendant 15 jours, éventuellement aidée d’une infirmière les premiers jours.
Le soutien gorge de contention est à garder en permanence jusqu’à 3 semaines après l’intervention.
Combien de temps il faut porter un soutien-gorge après une réduction mammaire ?
Le soutien gorge de contention après une réduction mammaire est à garder en permanence jusqu’à 3 semaines après l’intervention.
Réduction mammaire bonnet : Quel va être mon bonnet après l’intervention ?
La majorité des patientes nécessitant une réduction mammaire ont un bonnet supérieur au E.
Afin de conserver un galbe du sein harmonieux, il est nécessaire de garder un volume mammaire équivalent à un bonnet C.
Certaines femmes souhaitent un bonnet B, mais elles doivent être prévenues que les seins risquent d’être un peu plats et moins esthétiques.
Réduction mammaire et allaitement : Peut-on allaiter après une réduction mammaire ?
Grâce à la technique que nous pratiquons ( technique à pédicule supéro-interne), l’allaitement est possible après une réduction mammaire, ce qui n’est généralement pas le cas avec une technique classique à pédicule supérieur. La technique classique sépare l’aréole de la glande sous-jacente et les canaux galactophoriques amenant le lait sont coupés, c’est la raison pour laquelle nous avons décidé de ne plus réaliser cette technique.
Réduction mammaire Prix : combien coûte une réduction mammaire ?
L’assurance maladie prend en charge les réductions mammaires dont la pièce de résection glandulaire est supérieure à 300g par sein opéré.
Cela correspond en pratique à un gros bonnet D et au delà.
Dans ces cas, nous pratiquons des honoraires complémentaires qui varient entre 3500 à 4000 euros, pouvant éventuellement pris en charge par votre complémentaire santé.
Si la résection glandulaire prévue est inférieure à 300g, les prix d’une réduction mammaire correspondent à ceux d’une cure de ptôse simple esthétique (de 7500 à 9000 euros)
Réduction mammaire prise en charge : un remboursement possible ?
Une réduction mammaire peut être prise en charge par l’Assurance Maladie sous certaines conditions. Pour bénéficier d’un remboursement d’une réduction mammaire, l’intervention doit permettre de retirer au minimum 300 grammes par sein, critère indispensable pour que l’opération soit considérée comme réparatrice et non esthétique. Cette évaluation est effectuée lors de la consultation avec votre chirurgien plasticien.
A noter que les honoraires complémentaires restent à la charge de la patiente et peuvent éventuellement être remboursés par votre complémentaire santé.
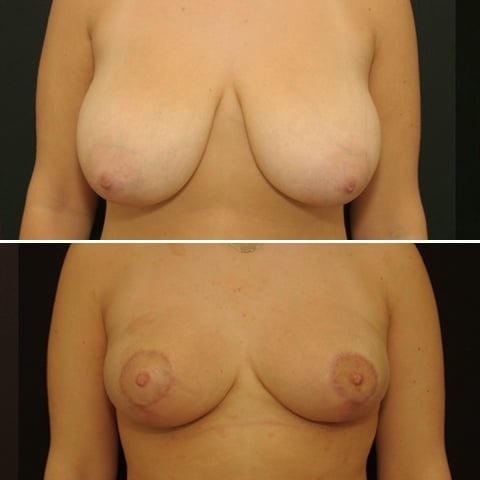
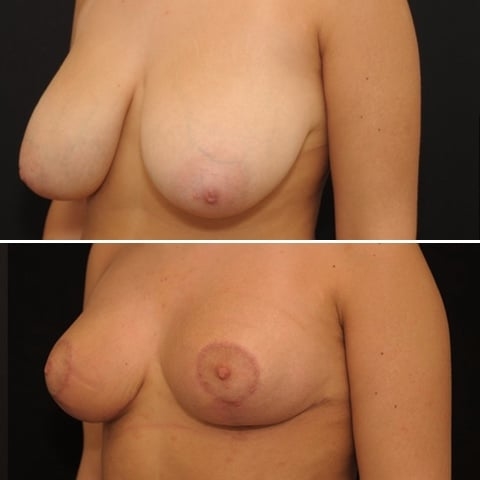
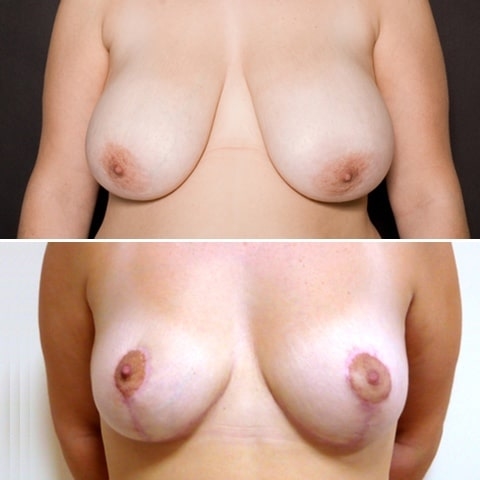
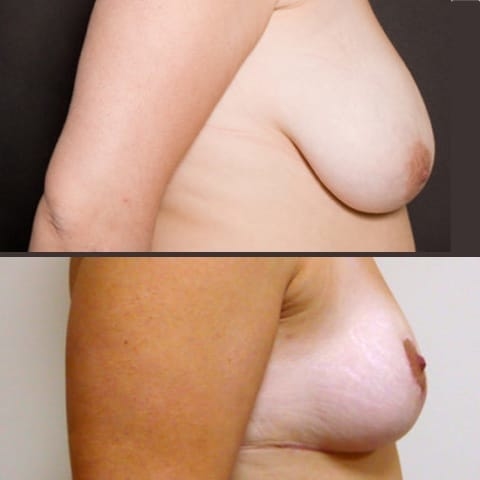
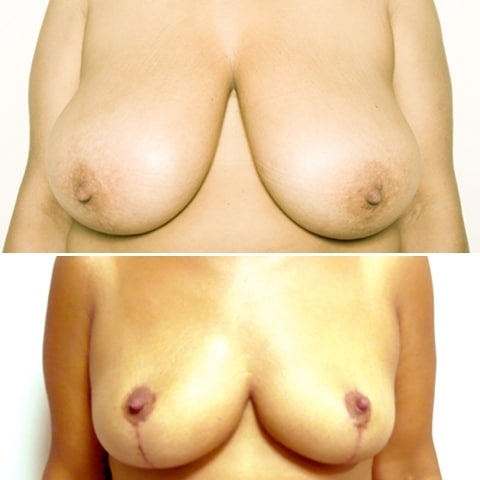
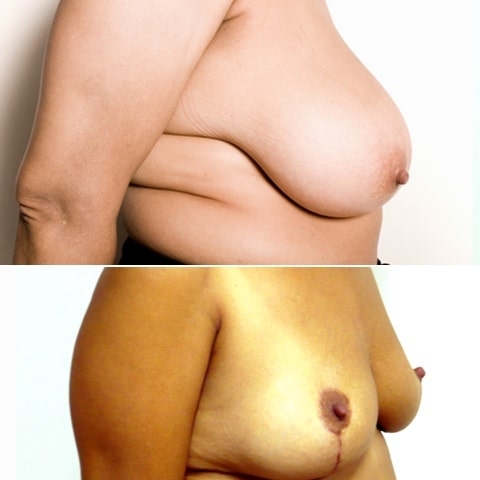
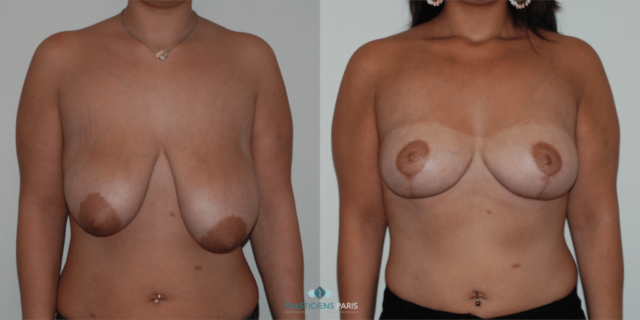
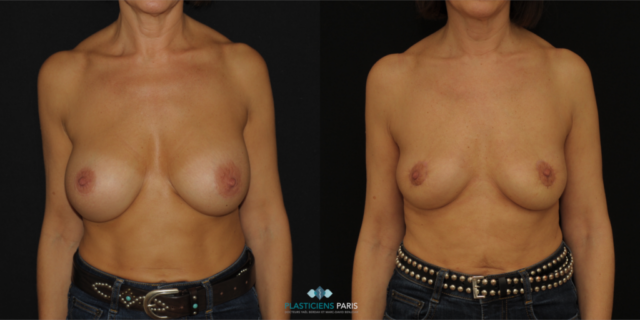
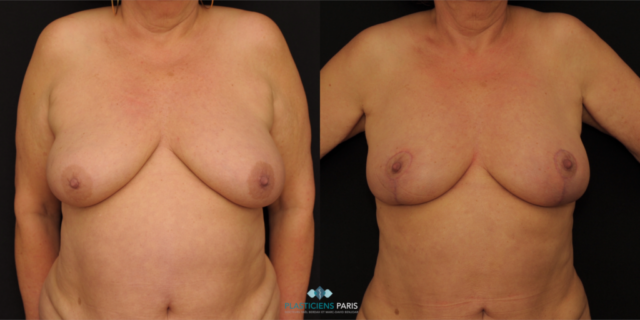
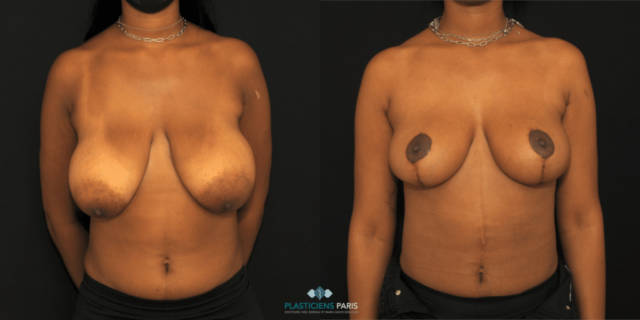
Réduction mammaire avant après : photos d’une diminution des seins
Découvrez les photos des résultats d’une réduction mammaire avant après, intervention réalisée par le Dr Benjoar et le Dr Berdah, chirurgiens mammaires à Paris depuis plus de 15 ans.
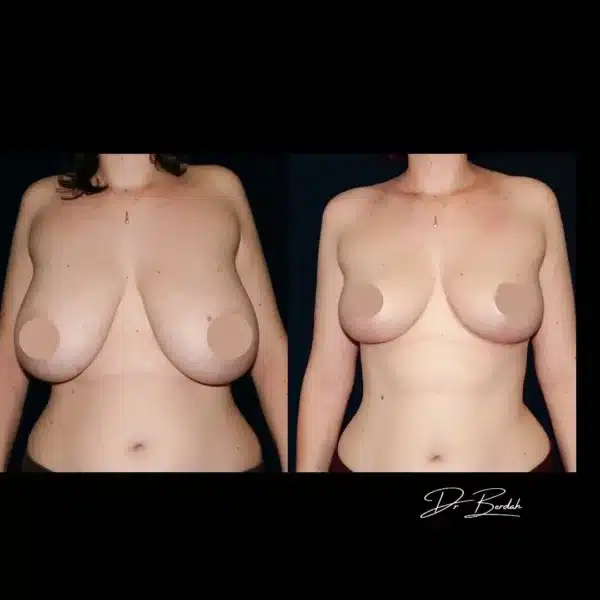
Réduction mammaire bonnet F avant après
Découvrez les résultats d’une plastie de réduction mammaire d’un bonnet f avant après avec cicatrices en T inversé après un retrait de 700 grammes par sein. Photo à 6 mois.
Une question ? Contactez-nous !
Le cabinet de chirurgie esthétique à Paris
Docteur Yaël Berdah et Docteur Marc-David Benjoar
Chirurgiens esthétiques à Paris France